Feeling dizzy can be genuinely unsettling.
Sometimes it’s a brief spinning sensation when you roll over in bed. Other times it’s a lingering “off” feeling, unsteadiness on your feet, nausea, or a sense that you can’t trust your balance when you turn quickly, walk in crowds, or move your head.
The tricky part is that “dizziness” is a broad word. It can describe vertigo, imbalance, lightheadedness, or a mix of all three. Because of that, the most important first step is working out what type of problem you’re dealing with.
At PhysioCentral in Miranda, we assess and treat vertigo, dizziness and balance problems for people across the Sutherland Shire, with a strong focus on getting the cause right before building the right treatment plan.
What you need to know
The vestibular system is your body’s balance system. It sits mainly in the inner ear and works with your eyes, muscles, and joints to help you sense movement, keep your vision steady, and maintain balance.
Vertigo and dizziness are often linked to the vestibular system, with BPPV (Benign Paroxysmal Positional Vertigo) being one of the most common causes. BPPV typically causes brief spinning when you roll over in bed, sit up, bend over, lie down, or look up.
Other common presentations include post-viral vestibular problems, vestibular migraine, Ménière’s disease, post-concussion dizziness, neck-related dizziness such as cervicogenic dizziness, and longer-lasting dizziness that leaves you feeling off or motion-sensitive.
Not all dizziness is vestibular, though. If symptoms mainly happen when standing and improve when lying down, blood pressure or autonomic factors may also need to be considered.
If dizziness comes with a severe headache, weakness, trouble speaking, double vision, fainting, or sudden severe difficulty walking, seek urgent medical care.
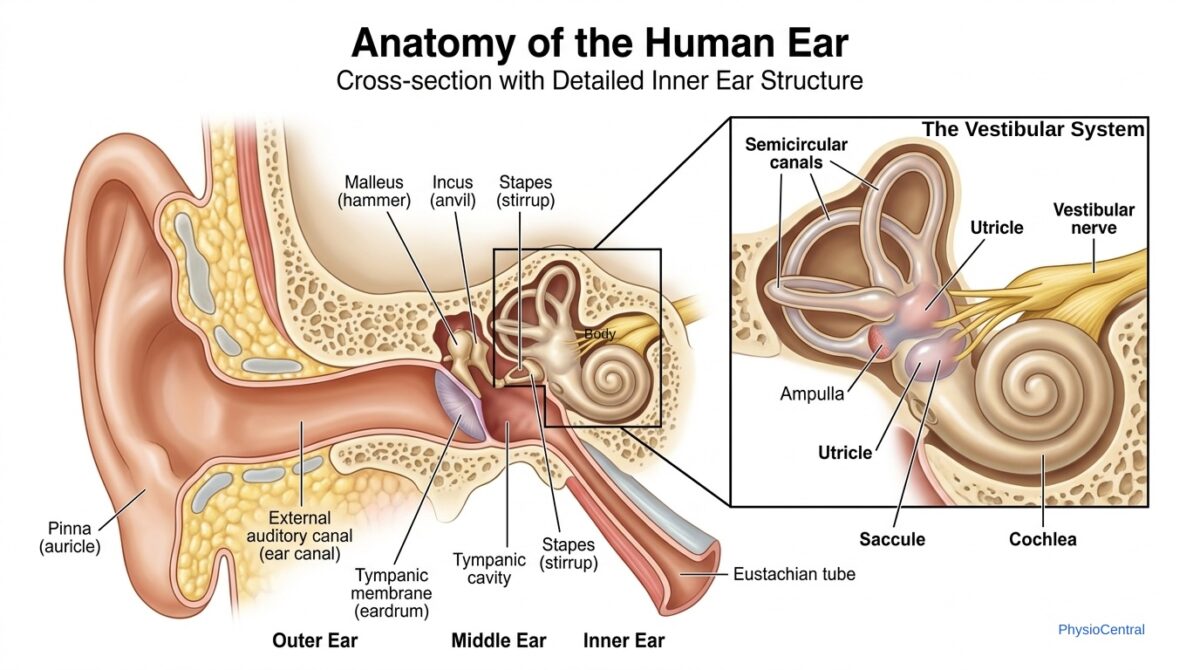
Where is The Vestibular System
The vestibular system is part of the inner ear. It helps your brain detect head movement and position, and works with your eyes and muscles to keep your vision steady and your balance under control.
On this page
- What you need to know
- Symptoms: what vertigo and dizziness can feel like
- What does the dizziness feel like? A quick guide
- When to get it checked
- Warning signs that need urgent medical care (Red Flags)
- What to do at home in the early phase
- How we assess vertigo and dizziness at PhysioCentral
- Treatment that works: our Diagnose, Treat, Retrain, Return framework
- Common vertigo and dizziness conditions we treat
- FAQs
- Vertigo and dizziness treatment in Miranda
Symptoms: what vertigo and dizziness can feel like
Vertigo and dizziness aren’t always just “spinning”. People often describe:
- spinning or the room moving
- unsteadiness, veering, or feeling wobbly while walking
- nausea or vomiting
- feeling worse with head movement, rolling in bed, getting up, bending over, or looking up
- feeling “off” in supermarkets or visually busy environments
- reduced confidence walking, especially in low light or on uneven ground
- feeling like quick turns, crowds, or head movement bring symptoms on
What does the dizziness feel like? A quick guide
This section isn’t a diagnosis, but it can help connect what you’re feeling with the kinds of presentations we commonly see.
- Brief spinning when rolling in bed, sitting up, looking up, or bending: often BPPV
- A major dizzy episode after a virus, followed by lingering imbalance: often post-viral vestibular problems
- Episodes with a migraine history or strong motion sensitivity: often vestibular migraine
- A persistent “off” feeling, worse in busy environments: often persistent dizziness, including PPPD (Persistent Postural-Perceptual Dizziness) – style presentations
- Ear fullness, tinnitus, or hearing changes with vertigo episodes: may fit a Ménière’s-type presentation
- Lightheadedness on standing, better when lying down: may reflect an orthostatic or autonomic issue
- Dizziness with neck pain, stiffness, or symptoms brought on by neck movement: may reflect cervicogenic dizziness, especially if the neck seems to be part of the problem
🔍 When to get it checked
It’s worth getting assessed if:
- symptoms are lingering beyond a couple of weeks
- dizziness keeps returning with normal daily movement
- rolling in bed, looking up, bending, walking in crowds, or turning quickly keeps bringing symptoms on
- you’re losing confidence with walking, driving, shopping, or training
- symptoms are interfering with work, exercise, or day-to-day life
🚩Warning signs that need urgent medical care (Red Flags)
Most dizziness and vertigo episodes are not dangerous, but some symptoms can point to something more serious and should not be ignored. Seek urgent medical care straight away, or call 000 for an ambulance, if dizziness or vertigo comes with any of the following:
- a new, severe, or unusual headache
- double vision, sudden vision loss, or major visual disturbance
- trouble speaking or swallowing
- weakness, numbness, facial droop, or difficulty lifting an arm
- fainting, seizures, or confusion
- sudden severe difficulty walking, repeated falls, or being unable to stand
- ongoing vomiting or rapidly worsening symptoms
Use the FAST rule if stroke is a possibility:
- Face drooping
- Arm weakness
- Speech difficulty
- Time to call 000
Even if these symptoms improve quickly, they still need prompt medical assessment.
What to do at home in the early phase
If you’re dizzy today, the first priority is safety.
It often helps to:
- move slowly when changing position
- use handrails or support if you feel unsteady
- avoid ladders, heights, and risky environments
- avoid driving if you don’t feel safe to drive
- reduce sudden repeated head movements until you know what’s triggering symptoms
- focus on hydration if symptoms are mainly happening when you stand up
How we assess vertigo and dizziness at PhysioCentral
A good vestibular assessment is structured and specific. We’re not just asking whether you feel dizzy. We’re working out what type of dizziness you have, what triggers it, and what needs to happen next.
We typically look at:
- your symptom history and the movements or situations that bring symptoms on
- whether the problem feels more like vertigo, imbalance, or lightheadedness
- eye movement findings, because the vestibular system and eye control are closely linked
- positional testing for BPPV, including which side and which canal may be involved
- standing and walking balance
- head movement tolerance during functional tasks
- a neck-related dizziness presentation, including cervicogenic dizziness
- signs that the issue may be non-vestibular and needs GP or specialist review
We’ll also give you a clear home plan, including what to work on, what to avoid for now, and when to seek further review.
Practical tip: people can occasionally feel temporarily worse after testing or treatment, especially if BPPV is triggered during the appointment. If you don’t feel safe driving when symptomatic, it’s sensible to arrange a lift for the first visit.
What works: Diagnose – Treat – Retrain – Return to normal
Vertigo and dizziness usually improve best when treatment follows a clear sequence.
Phase 1: Diagnose
The first step is identifying the main cause.
We’re working out whether your symptoms best fit:
- positional vertigo, often BPPV
- a post-viral vestibular issue
- migraine-related dizziness
- a persistent dizziness presentation
- post-concussion dizziness
- a non-vestibular lightheadedness issue
This matters because the right treatment depends on what’s actually driving your symptoms.
Phase 2: Treat
Once the main cause is clearer, treatment is matched to that problem.
If BPPV is present, treatment is canal-specific repositioning. It isn’t just one manoeuvre for everyone.
The inner ear has three semicircular canals, each with a different positioning treatment required. We can accurately determine which canal is affected and apply the appropriate treatment, as well as prescribing the best home exercise program to follow.
If the cause is something else, treatment may focus on:
- gaze stability retraining
- habituation, using gradual exposure to movements that trigger symptoms
- balance retraining
- walking retraining
- reducing fear and avoidance around movement
Phase 3: Retrain
As symptoms become less reactive, we build tolerance to normal movement patterns back up step by step. We often refer to this as Vestibular Rehabilitation.
This may include:
- head movement while walking
- turning, changing speed, and changing direction
- visual challenge in busier environments
- balance tasks that add in scanning, talking, or other real-world demands
Phase 4: Return
The final stage is getting back to normal life with more confidence.
That may include:
- driving
- shopping
- work tasks
- training and sport
- social activity
- having a plan for what to do early if symptoms flare again
A simple visual guide to vertigo and balance disorders

Common vertigo and dizziness conditions we treat
BPPV (Benign Paroxysmal Positional Vertigo)
BPPV is one of the most common causes of vertigo. It usually causes brief spinning when you roll in bed, lie down, sit up, bend over, or look up.
It’s also commonly oversimplified. Different semicircular canals can be involved, and the correct manoeuvre depends on the canal affected and the test findings. If positional vertigo isn’t settling, keeps returning, or doesn’t match the usual story, it’s worth a proper vestibular assessment rather than repeating random manoeuvres.
After a more detailed look into the complexities of BPPV?

Read more about BPPV (Benign Paroxysmal Positional Vertigo)
Its causes, symptoms, and treatment here.
Post-viral vestibular issues
After a virus, some people are left with lingering dizziness, imbalance, nausea, and reduced tolerance to movement. These cases often improve with a structured vestibular rehab plan, but they usually need more than just “rest and wait”. Successful recovery needs to be active.
Vestibular migraine
Some people experience dizziness, vertigo, or strong motion sensitivity linked to migraine, sometimes even without a major headache. These cases often improve best when the migraine-related vestibular features are recognised early and rehab is matched appropriately.
Often also requires a thorough assessment of your neck.
Ménière’s-type presentations
Ménière’s disease can cause episodes of vertigo along with tinnitus, hearing changes, and a sense of fullness in the ear. These symptoms should be properly assessed so the right medical and rehab pathway is followed.
Persistent dizziness presentations
Some people develop a longer-lasting “off” feeling, motion sensitivity, or visual sensitivity, often worse in supermarkets or busy environments. These cases usually respond best to a calm, structured plan and consistent graded exposure.
Post-concussion dizziness
Dizziness and balance problems after concussion are common. Many improve with targeted vestibular and balance rehabilitation, especially when symptoms have lasted beyond the very early phase.
Cervicogenic dizziness
Some people feel dizzy, lightheaded, or unsteady in a way that seems closely linked to neck pain, stiffness, or neck movement. This is often described as cervicogenic dizziness.
It can be harder to diagnose than BPPV or other inner ear causes, because there isn’t one single test that confirms it. Instead, it is usually considered after other likely causes of dizziness have been ruled out. When the neck is a meaningful part of the problem, treatment may include addressing the neck itself as well as balance or vestibular rehabilitation where needed.
FAQs
What is the difference between dizziness and vertigo?
Vertigo usually feels like spinning or motion. Dizziness can also mean lightheadedness, unsteadiness, or a vague “off” feeling. Working out which one you’re dealing with helps guide the right treatment.
Why do I get vertigo when I roll over in bed?
That pattern is very common in BPPV, where brief vertigo is triggered by changes in head position such as rolling, sitting up, lying down, or looking up.
Can physio help vertigo and dizziness?
Yes. Many vestibular conditions respond well to physiotherapy, including canal-specific treatment for BPPV when appropriate, as well as vestibular rehabilitation to improve gaze stability, balance, and movement tolerance.
My dizziness has lasted for weeks. Does that mean it’s serious?
Not necessarily. Ongoing symptoms can happen for several reasons, including post-viral changes, migraine-related dizziness, persistent dizziness, or reduced movement confidence. It’s still worth a proper assessment so you know what’s going on and what to do next.
Could dizziness be related to blood pressure?
Yes. If symptoms mainly happen when standing and improve when you lie down, it may reflect an orthostatic or autonomic issue. That’s worth discussing with your GP alongside physio assessment.
When should I worry about stroke?
If dizziness comes with FAST signs (mentioned above), sudden severe headache, double vision, fainting, marked weakness, or major difficulty walking, please call 000.
Vertigo and dizziness treatment in Miranda
If you want help understanding the cause of your dizziness and following a practical treatment plan, our vestibular physios, Graeme and Jack, at PhysioCentral in Miranda, can help.
We’ll assess what’s most likely causing your symptoms, guide you to the right treatment first, and help you rebuild confidence with a clear plan to return to your normal daily movement.